Health Benefits Questions
"Your health care benefits…at a glance."
This is a listing of the questions & replies that have appeared in AREA's Newsletter. We obtain the information from the AAFES Benefits section.
Health Benefits Questions (click on questions for answers)
- How did employer sponsored health plans get started?
- How is health care managed in AAFES?
- What's the AAFES Benefits Chain-of-Command for health benefits issues?
- We heard that you revised the way to determine what plan of benefits applies when a retiree (or spouse) is eligible for Medicare and the other person is not?
- What's the value of the AAFES post-retirement medical benefit and access to group rates through AAFES' Long Term Care (LTC) Plan?
- How are employee contributions to the pension plan paid out to the retirees? (This is the small part of the annuity that's not taxable.)
- Does the PPO Dental Plan work in the same way as the PPO Medical Network?
- What should I do when "I reach that age"?
How did employer sponsored health plans get started?
Employers first started offering health plans in response to their inability to increase pay. Pay caps were common during WW II, so employers added benefit packages instead. At that time, traditional health plans were intended to only cover catastrophic illnesses or injury. Then came initiatives by employers to cover cancer-prescreening tests, and eventually routine preventive exams / tests were covered. Dental was subsequently added as a minor benefit program. In fact, many employers still do not offer very strong dental benefits because the thought is that someone is not going to lose their house over a dental claim as you would for cancer, transplant, etc. Also in the early days, there was a flat medical inflation trend, so employers did not have to worry about impact of health care costs on their financial results, as is the situation today.
These past trends, coupled with employees experience with no deductibles and / or low co-pays through managed care, left many employees feeling that benefit programs had made the transition from covering catastrophic costs to being an entitlement covering all or most of the costs. The reality is that this view is simply not sustainable in an environment of rapidly increasing medical costs and aging baby boomers. Benefit participants oftentimes view doctor visits as costing the $15 or $25 co-pay price when, in reality, that is only a small part of the health care cost. Additionally, Rx commercials have a cost-invisible orientation that causes many people to believe that they can be acquired at no or nominal cost.
The rapid pace of medical and economic changes these past several years have left the impression that there has been an erosion of benefits compared to earlier periods. Actually, plan participants pay significantly less now than before, even with the benefit changes. For example, in 1960, out of every dollar spent on healthcare, the consumer paid an average of 60 cents and the employer (the plan) paid about 40 cents. Today, the participant pays only about 14 cents out of that same dollar of health care cost. The current trend in employer health plans is to encourage participants to become wise healthcare consumers by making sure they understand the real cost of healthcare and engaging them in making more cost effective decisions. Typically, that means higher co-pays.
How is health care managed in the Exchange?
The Exchange manages health care benefits and their costs through the Associate Total Compensation Committee (ATCC). The Committee reviews all pay and benefit changes for active and retired associates. Both the financial Management & Accounting Directorate (FA) and the Human Resources Directorate (HR) submit agenda items to this group. The Deputy Commander is the Committee Chairperson, and a voting member. Other voting members are the COO and Senior Vice Presidents (SVP) of FA and HR. The SVP, Management Information Systems Directorate (IS) is the "at large" member. The Office of the General Counsel (GC) advises the Committee as a non-voting member. Any change to the Department of Defense, Non-Appropriated Fund (DOD NAF) plan applies equally to active and retired participants. That is, we all have the same coverage levels depending on which plan applies to us based on zip code and whether or not the retiree is eligible for Medicare. Since retiree and active claims are "pooled," the premiums established take into consideration claims for all participants, not just active employees.
The ATCC is responsible for determining the Exchange position and "vote" on the DoD NAF Health Benefits Program Committee (HBPC). There are six voting members (one from each NAF). A representative from the DoD Civilian Personnel Policy (CPP) office chairs the Committee. The Committee makes recommendation to the Undersecretary of Defense regarding premiums and plan changes to the DOD-NAP Plan.
Here is a summary of the HBPC process. One of the NAFs or Aetna makes a recommendation to change a plan provision. Typically, Aetna will be asked to give the Committee an estimate of what it would cost the plan, when it is a benefit improvement, or what it would save the plan, if the change involved higher co-pays, etc. The committee considers the impact on employer costs, the benefit to the participants and other factors. The Committee reviews all information, including what other employers are doing, what civil service employees have as a benefit, and what our benefit consultants recommend. Based on this information, the NAF members return to their respective organizations and make a recommendation on the proposal.
In the Exchange, agenda items are forwarded to the ATCC, with a recommendation on the Exchange position on the benefit changes. Once votes are gathered and coordinated with the Commander's office, the Exchange vote is forwarded to the DoD. Based on a majority vote, the HBPC Committee recommendation is adopted or rejected. If the proposal is adopted, DoD sends a recommendation to the Undersecretary of Defense to make the change to the Plan or, if a premium adjustment is necessary due to projected medical trend, what percent increase the premium should be. If the vote of the committee is tied 3 / 3, typically DoD CPP will send the matter to the heads of the components, i.e., the Dept. of Army, Dept. of Air Force, Dept. of Navy (NEXCOM = Navy Exchange; BUPERS - Bureau of Personnel, and Marine Corps) and the Commander, the Exchange for comment / position. A decision is then made on the proposed change, based on the component votes.
What's the Exchange Benefits Chain-of-Command for health benefits issues?
The Exchange is a member of the DoD NAF HBP (Health Benefits Plan) so the chain-of-command is related to that program. Here's the process to follow for the quickest and most assured resolution of health benefits issues.
1. Initial contact: Aetna, including their internal appeal process on claims denials.
2. Next level of contact: The Exchange Benefits Technician to make a general complaint about Aetna's performance or for assistance in resolving the issue. The Exchange Benefits Office phone # is (800) -519-3381. You can also send your inquiry to benefits@aafes.com.
3. You may send a formal appeal in writing to the Plan Administrator. According to DoD policy, the Plan Administrator has final decision authority on appeals. Please send to:
AAFES HQ
FA-T Benefits
P O Box 650428
Dallas TX 75265
The Exchange advocates health care issues on behalf of its Associates and Retirees. Along with the DoD Civilian Personnel Policy Office and other NAFs, AAFES regularly meets with Aetna to resolve claims issues, determine plan designs changes, improve customer service and work on other key items of interest. In the DoD contract with Aetna, performance guarantees are in place for claim accuracy, turnaround time on claim processing, participant satisfaction and other areas of high concern.
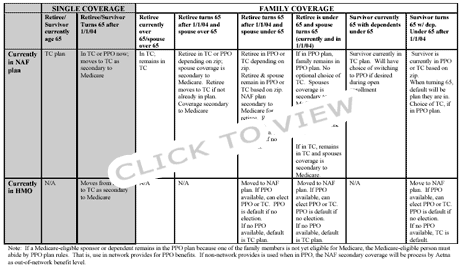
We heard that you revised the way to determine what plan of benefits applies when a retiree (or spouse) is eligible for Medicare and the other person is not?
Yes, we did. Here's the current chart. Changes allow for all participants to stay in the PPO plan until the whole family reaches age 65. This allows you to take advantage of copays; however, you are required to file with Medicare first. Changes allow the spouse that is Medicare eligible to remain in the same medical plan as the sponsor and to take advantage of copays; however, the spouse is required to file with Medicare. We also added the rules for the surviving spouse and split families.
Note: Dental coverage is not affected by Medicare eligibility.
Another Job After Retirement? If you work somewhere after retirement and enroll in insurance at that workplace: THAT coverage becomes primary, THEN secondarily would come the Medicare coverage and / or the Exchange, as shown above.
Reason: Insurance coverage from a workplace where you receive wages (as opposed to a pension) will always be the most primary coverage.
What's the value of the Exchange post-retirement medical benefit and access to group rates through AAFES' Long Term Care (LTC) Plan?
Look at your own expenses for medical and LTC benefits and compare to the following information.
- Fidelity researchers estimate that a couple retiring today at age 65 who do not have access to employer-paid retiree medical insurance would have to have saved about $160,000 to cover Medicare premiums, expenses associated with Medicare cost-sharing provisions and services not covered by Medicare. The costs of long-term care, except on a very limited basis, would add $130,000 to the needed savings.
- But many employees actually retire earlier than 65. Since costs in the individual insurance market regularly tally at least $10,000 every year for two-party coverage, a couple retiring at 60 would need more than $200,000 to pay for anticipated expenses, $330,000 if long-term care is taken into account.
- Many large employers, if they continue to offer retiree medical benefits at all, usually limit their liability by capping benefits during one's lifetime (usually at $ .5M or $1M). The DOD NAF health plan protects all associates and retirees by providing unlimited lifetime coverage.
How are employee contributions to the pension plan paid out to the retirees? (This is the small part of the annuity that's not taxable.)
This is best illustrated by an example. Our EXAMPLE assumes both the retiree and spouse are 55 years old, with an annuity start date of December 2002, and includes a spousal annuity:
The amount of your benefit that is attributable to the employee contributions is determined according to the Internal Revenue Code Simplified Method of Taxing Annuity Payments Sec 72(d)(1)(B). The number of anticipated payments is determined according to an actuarial table set forth by the IRS. The life expectancy used in these tables for a single life is assumed to be on average 82 and for joint lives is assumed to be on average 86.
The calculation is based on a factor of 410 anticipated monthly payments because the retiree elected the Joint and Survivor annuity. This assumes that the life expectancy is about 34 years (i.e. 410 / 12), or age 89 (i.e. 55+34) for the combined lives since both are on the younger end of the table. The employee contributions without interest is then divided by 410 to arrive at the non-taxable portion of the monthly benefit. Therefore, the calculation in this example = 57754.05 / 410 = $140.86. This is the amount that shows up as the EECONT source on the monthly pension check.
Additionally, according to Section 72(b)(3) of the IRS Code...(paraphrasing the actual code) "Where annuity payments cease before the entire investment (contributions without interest) is recovered.... The amount of such unrecovered investment shall be allowed as a tax deduction to the annuitant for his last taxable year."
Does the PPO Dental Plan work in the same way as the PPO Medical Network Plan?
No, it doesn't. Let me explain. The PPO dental plan benefit levels for in- and out-of-network are the same and there is no penalty for using an out-of-network dentist. The fact that Aetna has only a few PPO dentists in a certain area is one of the reasons the DoD NAF Committee decided to make the PPO dental plan completely voluntary. The out-of-network benefits are the same benefits provided under the old Traditional Choice dental plan so there is no penalty for going out of network.
Participants who live in areas where access to PPO dentist is available are encouraged to use them. Why? Using an in-network dentist can save you significant dollars because the rates charged are always within the prevailing fee limit so you don't have any unexpected out-of-pocket costs. Some participants have told us that they have saved as much as $500 or more a year depending on what procedures they have done. The PPO dental plan also allows you to stretch your dental benefits further since the percentage coverage applies to a lower total cost. This in turn helps participants stay under the $2,000 annual dental benefit maximum. Again, the choice to use an in-network dentist is completely up to you. We've had nothing but enhancements to the dental plan in the last several years.
On the other subject of PPO medical plan benefits for under 65 spouses of Medicare eligible retirees.... this would be a positive benefit change for the majority of participants. Aetna's PPO networks have grown significantly over the last few years in all but a few rural locations. In areas where the network is not adequate, we've asked participants to provide us evidence of that fact. If justified, we will approve on a case-by-case basis keeping
participants in a particular zip code in the Traditional Choice plan. This is not a permanent exemption as networks change yearly. There is no reason for a participant to unilaterally use all out-of-network doctors unless they simply want to retain a relationship with particular out-of-network physicians only and are willing to incur the added out of pocket costs associated with the non-network benefit level. Based on reports we receive
from Aetna, very few people make that choice.
What should I do when "I reach that age"?
Here are the various steps you have to take to sign up for Social Security and Medicare, when your AAFES life insurance decreases and how your 401 (k) funds are administered.
AGE |
What Happens |
What YOU need to do |
|---|---|---|
62 |
Most retirees can: Begin Social Security payments at 62, OR Wait a few years to begin, in exchange for a larger amount. If you retired early (under age 62), AAFES is paying you an estimated Social Security 'bridge' payment as part of your pension, in addition to your normal / basic pension amount. The Exchange will always stop paying the 'bridge' amount at age 62, whether your real Social Security begins at 62 or later. That means your total pension check will decrease, but your Social Security payments should make up the difference (and possibly more). |
On your State Street pension stub; "SS LEVEL" is the estimated Social Security bridge amount that AAFES has been paying you. Visit your Social Security office. Find out how much you'll receive at 62, versus the amount available if you wait a few years. Can you wait? Immediately after you begin, compare the real Social Security payments to the "SS LEVEL" that AAFES had been paying. Which one is higher? If "SS LEVEL" is higher, call HQ Benefits within 90 days at (800) -519-3381. You may be eligible for a higher basic pension! |
65 |
Most people are eligible for Medicare at 65, and if so, that will now become your primary coverage. If you qualified to keep your health coverage for life, you'll still keep it, but it is now secondary to Medicare. Also: if it wasn't already, the type of plan will change to be Traditional Choice. If this is a change for you, you'll get new insurance ID cards in the mail for this secondary coverage. |
Sign up at your local Medicare office BEFORE your 65th birthday, and check on the monthly cost. Learn how it works with any other medical coverage you have. Ask about Medicare HMOs available in your area, and what their premiums are. Show your Medicare card to doctors first, since it's your primary coverage now. Ask Aetna about Medicare Direct, to reduce your medical claims paperwork. |
66 |
If you qualified to keep your Life Insurance, the value* will now reduce (the first time) at age 66, by 25 percent. * The value at retirement was equal to your salary at retirement, times two. |
Call the Exchange Benefits at (800) -519-3381 within 31 days of turning 66, if you want to convert some of that 'reduced' value to an individual plan. |
67 |
If you retired and qualified to keep your Life Insurance, the value will now reduce (a second time) at age 67, by another 25 percent. This makes a 50 percent reduction since retirement. |
Call the Exchange Benefits at (800) -519-3381 within 31 days of turning 67, if you want to convert some of that 'reduced' value to an individual plan. |
68 |
If you retired and qualified to keep your Life Insurance, the value will now reduce (a third and final time) at age 68, by another 25 percent. This makes a 75 percent reduction since retirement. |
Call the Exchange Benefits at (800) -519-3381 within 31 days of turning 68, if you want to convert some of that 'reduced' value to an individual plan. |
70.5 |
The Exchange 401(k) Retirement Savings Plan was amended in 2002 to allow retired employees and retired employee surviving spouses who have reached 70 1 / 2 to remain in the plan. |
|
73 |
For the Exchange 401(k) Retirement Savings Plan, you must start taking a Required Minimum Distribution (RMD) at 73. |
Call Fidelity at (800) 835-5098 to set up your RMD or rollover the total balance to an IRA. |







 Deals
Deals Clearance
Clearance Unit Purchases
Unit Purchases Marketplace
Marketplace Weekly Ad
Weekly Ad